
To understand the hemorrhoid banding procedure, it first helps to know how hemorrhoids form. Hemorrhoids can develop any time a person puts too much pressure on the veins in the rectal area. For example, during a bowel movement, the anal tissue fills with blood to aid the process. If you strain during a bowel movement, you may increase pressure in anal veins, causing these veins to swell or stretch. Usually, this swelling resolves quickly after straining, but sometimes the tissue remains engorged. The swollen tissue is called a hemorrhoid.
Other factors that may cause too much pressure to build include:
The risk of developing hemorrhoids also increases if you are between 45 and 65 years old. However, hemorrhoids can happen at any age, and it’s not uncommon for young people to experience hemorrhoids. Most people will have a hemorrhoid at some point in their life.
Fortunately, today’s patients do not have to live with the discomfort of having hemorrhoids, nor do they have to choose surgery to find relief.
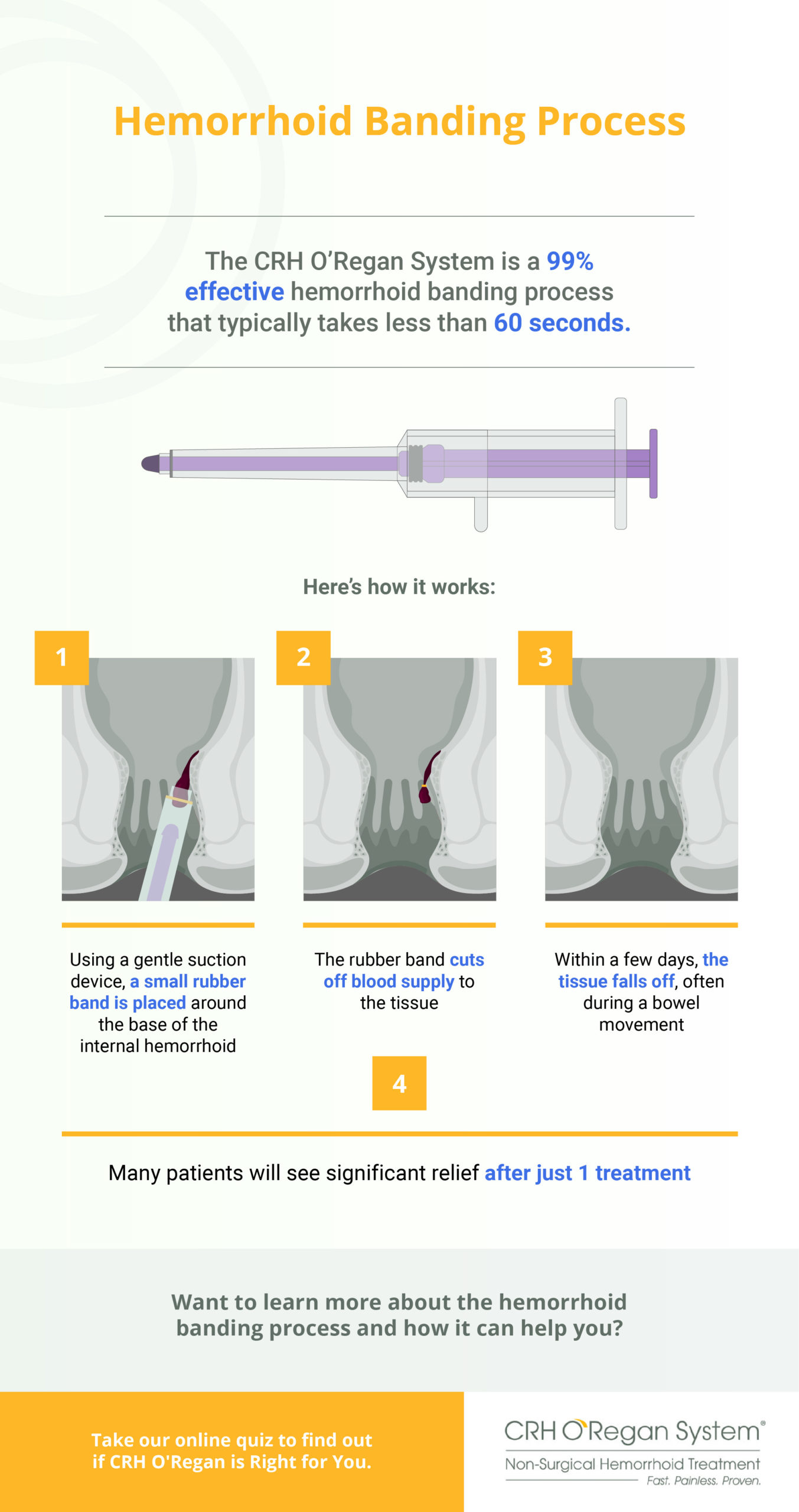
Hemorrhoid banding, or rubber band ligation, is a painless, minimally invasive method used to treat internal hemorrhoids and relieve external hemorrhoid symptoms.
According to an article published in the World Journal of Gastrointestinal Surgery, rubber band ligation is one of the most commonly used and cost-effective treatments for internal hemorrhoids. In this chapter, we’ll show you how internal hemorrhoid banding works.
Humans have been treating hemorrhoids for thousands of years. Before the invention of rubber band ligation, physicians used a range of methods to relieve hemorrhoid symptoms, including various surgical and ligation techniques. For example, during the fifth century B.C., Hippocrates wrote about a procedure similar to rubber band ligation, which involved tying hemorrhoids with a thick woolen thread “until they drop off.”
It wasn’t until the 1950s that Paul C. Blaisdell first described rubber band ligation as we know it today. The procedure was based on Blaisdell’s idea that internal hemorrhoids are easy to access and have few pain-sensitive nerve endings. Due to the procedure’s simplicity, doctors could use rubber band ligation to provide hemorrhoid treatment in their office rather than in a hospital.
Then, in the 1960s, J. Barron modified outpatient hemorrhoid ligation by using rubber bands and a device called the Barron band ligator. The Barron hemorrhoid ligator is a metal device that uses forceps to grasp the hemorrhoid before placing a rubber band around its base. Since Barron’s technique, various types of forceps have been invented to perform rubber band ligation.
Even though Barron’s ligation method is generally considered simple and safe, it needed improvement. Doctors found that grasping the hemorrhoid with forceps wasn’t always easy and could cause post-procedure pain.
In 1997, laparoscopic surgeon Dr. Patrick J. O’Regan improved hemorrhoid banding instruments by inventing a painless suction device called the CRH O’Regan ligator. Doctors can use the CRH O’Regan ligator to safely band hemorrhoids within seconds in their own office, and without the patient experiencing any pain.
Today, over a million rubber band ligations have been performed using CRH O’Regan technology.
When a doctor uses a ligator to place a tiny elastic band around a hemorrhoid, it cuts off the hemorrhoidal tissue’s blood supply. This causes the hemorrhoid to painlessly wither and fall from the living tissue in about a week. The surrounding tissue then forms a small scar as it heals. Once a scar forms where the hemorrhoid used to be, it helps keep hemorrhoids from coming back in the same spot.
Your doctor may recommend rubber band ligation to treat hemorrhoids that are prolapsed or causing symptoms such as:
Hemorrhoids can become itchier or more painful over time if they remain untreated. Any patient who suffers from recurring hemorrhoid symptoms might consider hemorrhoid banding.
Physicians can use several techniques and specialized tools to perform hemorrhoid banding. For example, ligators feature variations in the grip. Some ligators have a pistol grip, while others feature a scissors grip. The mechanisms for capturing the hemorrhoid and releasing the band also vary.
Even though the following procedures all aim to ligate hemorrhoids, they may produce different results since they involve distinct devices and techniques. Here are the various types of hemorrhoid banding:
During a traditional rubber banding hemorrhoid procedure, the doctor clamps the hemorrhoid with metal forceps and pulls it away from the anal wall. Next, the doctor places a rubber band around the hemorrhoid to cut off blood flow, causing it to dry up and eventually fall off. Traditional rubbing band ligation takes five to 10 minutes, and patients may require up to three days to recover.
This procedure usually causes post-procedure pain and bleeding, and physicians often prescribe pain medication to help patients get through their recovery. According to the World Journal of Gastrointestinal Surgery, pain is one of the most common complications of traditional rubber band ligation and occurs in about 25% to 50% of patients.
Endoscopic band ligation involves the use of an endoscope. An endoscope is a thin, flexible tube that a doctor can put tools in, such as forceps. Endoscopes used for hemorrhoid banding have been fitted with a plastic cap containing elastic bands. After the doctor inserts the endoscope into the patient’s anus, they will use a suction device or forceps to secure the hemorrhoid before placing the band around the base of the tissue.
Endoscopic banding is more complex and costlier than other types of ligation. Endoscopic banding also typically requires fasting, bowel preparation and sedation. Patients may experience pain after an endoscopic banding procedure.
The CRH O’Regan technique is similar to traditional hemorrhoid banding, except it is less likely to cause pain because it does not involve metal clamps.
For example, one study found that patients had higher pain scores immediately after a traditional banding procedure involving forceps ligation than those who underwent suction ligation. Less than 1% of patients experience significant pain or other complications with the CRH O’Regan System.
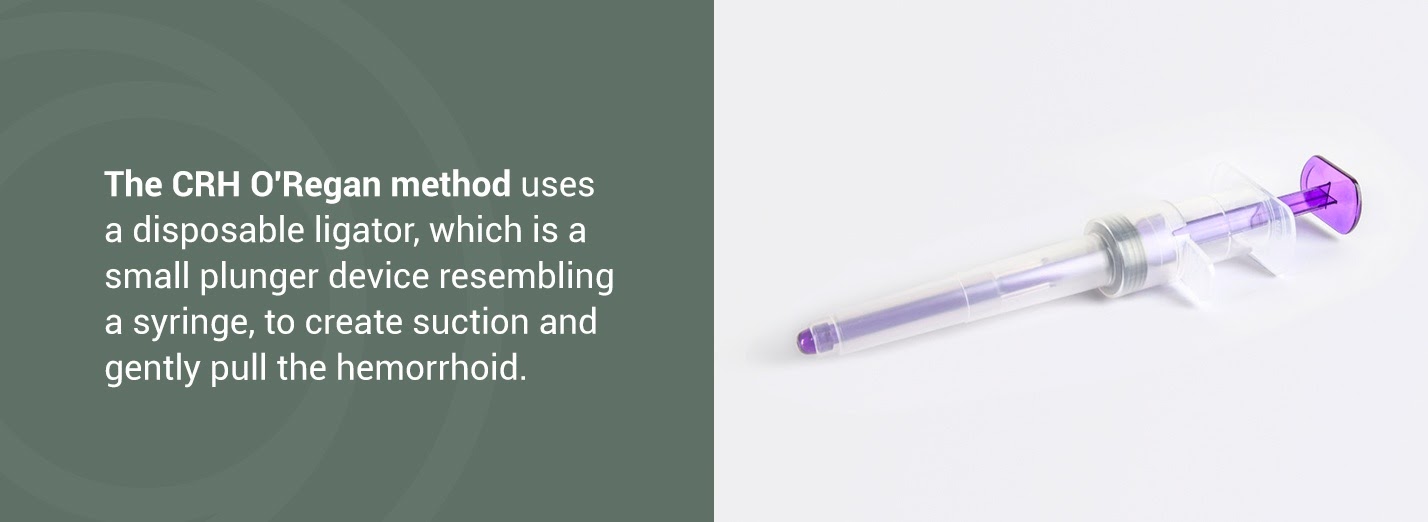
The CRH O’Regan method uses a disposable ligator, which is a small plunger device resembling a syringe, to create suction and gently pull the hemorrhoid. Once the hemorrhoidal tissue enters the device, a rubber band is released and placed around the tissue. There are no pain-sensing nerves where the doctor puts the rubber band.
Unlike other hemorrhoid banding treatments, the CRH O’Regan System does not require preparation, such as fasting or sedation. Nor does the doctor need to use any special instrumentation, and they can complete the treatment with only the CRH O’Regan ligator, examination gloves and lubricant. The procedure is also very fast and usually takes less than a minute, unlike other rubber band ligation procedures. Patients can undergo hemorrhoid banding with the CRH O’Regan System in their doctor’s office and return to work on the same day.
If you have multiple hemorrhoids that require treatment, your doctor will schedule a few more visits to perform the CRH O’Regan technique. Typically, your doctor will only place one band per visit to allow sufficient time for healing. Treating multiple hemorrhoids at once increases the risk of complications, so if possible, it’s worth it to undergo one treatment at a time.
Since there are three sites where hemorrhoids frequently form, most patients require a total of three treatments, with each appointment scheduled about two weeks apart. With Once you complete CRH O’Regan treatment, you can expect a low recurrence rate, similar to that of hemorrhoid surgery. Fewer than 5% of patients experience a recurrence within two years after CRH O’Regan treatment.
Hemorrhoid banding is not the only option for treating hemorrhoids, although it is highly effective and the most common procedure to remove internal hemorrhoids. Doctors may recommend other treatment methods if the hemorrhoids are too small or too large for rubber band ligation. Other hemorrhoid procedures include:
The surgical removal of a hemorrhoid is called a hemorrhoidectomy. During a hemorrhoidectomy, the doctor makes incisions in the tissue around the hemorrhoid and ties off the swollen vein inside the hemorrhoid to prevent bleeding. The doctor then removes the hemorrhoid and may or may not sew the area closed. They’ll then cover the wound with medicated gauze. Before undergoing a hemorrhoidectomy, the patient may receive general anesthesia to keep them from feeling pain.
Surgeons might use a scalpel, cautery pencil or a laser to perform a hemorrhoidectomy. This procedure is typically done in a surgery center or hospital. Patients can expect surgery itself to last 40 to 90 minutes.
Patients who undergo hemorrhoid surgery will need someone to drive them home from the procedure due to the effects of anesthesia. They’ll also need to eat a bland diet for a few days after surgery and use ice packs, warm-water baths and medication to relieve pain. In some cases, doctors give patients antibiotics to prevent an infection.
Hemorrhoid surgery is more expensive than hemorrhoid banding, involves a longer recovery time, has a higher risk of complications and is typically more painful. Some patients may need to stay in the hospital for a few days after the procedure due to pain, and overall, it can take over a month to recover. Doctors usually do not recommend a hemorrhoidectomy unless a patient has very large internal or external hemorrhoids.
Coagulation therapy, also known as infrared photocoagulation, uses heat to cut off the hemorrhoid’s blood supply. During this procedure, the doctor uses a device that creates a powerful beam of infrared light, which then heats the hemorrhoid. The process may take 30 seconds to three minutes.
Doctors might recommend coagulation therapy to treat small hemorrhoids that do not respond to home remedies. This procedure can be completed in a doctor’s office, and it may cause pain. The patient might also sense heat during the procedure. Coagulation therapy is expensive, and only one hemorrhoid can be treated at a time.
If patients have hemorrhoids that are too small for rubber band ligation, their doctor might suggest sclerotherapy. During sclerotherapy, the doctor injects the hemorrhoid with a chemical, which causes it to fall off eventually.
Patients commonly experience pain after undergoing sclerotherapy. Sclerotherapy also requires a high level of skill because if the doctor injects the substance into the wrong area, the patient can experience serious complications.
During cryosurgery, the doctor freezes the hemorrhoid with a cryoprobe and nitrous oxide or liquid nitrogen. In about three weeks, the hemorrhoid falls off.
Patients usually experience pain after cryosurgery, and there’s a risk of infection. Due to the increased complication risks related to this procedure, most doctors choose other forms of hemorrhoid treatment instead.
Stapling is a surgical technique used to treat large prolapsed hemorrhoids. During a stapling procedure, the doctor uses instruments to push the hemorrhoidal tissue back to its original location in the anal canal and staple it in place. The process may take anywhere from 15 to 90 minutes.
Although stapling is less painful than traditional surgery, it comes with a greater chance of recurrence, and it’s more expensive. Several complications are associated with stapling, such as the development of excessive scar tissue or trauma to the rectal wall.
Due to the complications associated with stapling and other surgical treatments, it’s worth confirming you need surgery with your doctor before moving forward. Hemorrhoid banding is much less invasive and just as effective as surgery.
Hemorrhoid banding is not considered surgery and does not involve incisions. Instead, hemorrhoid banding is thought to be the most effective non-surgical treatment for internal hemorrhoids.
External hemorrhoid banding is not effective. External hemorrhoids are located beneath the dentate line, where there are pain-sensing nerves, so they are too sensitive for banding.
Hemorrhoid banding is only used to treat internal hemorrhoids, which are located above the dentate line. However, if you treat internal hemorrhoids with the CRH O’Regan System, it can relieve swelling and symptoms associated with external hemorrhoids. Around 90% of patients with external hemorrhoid symptoms find relief with internal hemorrhoid banding. Protruding internal hemorrhoids may be mistaken for external hemorrhoids.

If you receive CRH O’Regan treatment, you will be awake during hemorrhoid banding. The CRH O’Regan System does not require sedation because it is fast, painless and can be done in a doctor’s office.
If you have more questions about hemorrhoid banding and how it works, please contact a CRH O’Regan Physician near you.